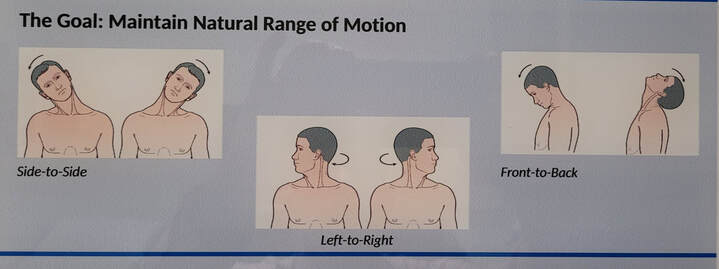
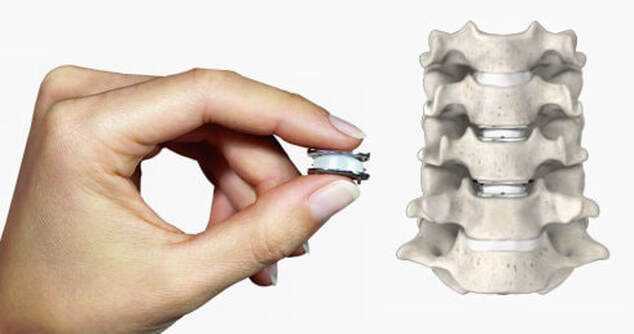
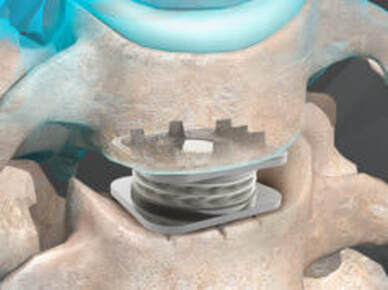
Things you should know about Disc Replacement Surgery:Disc replacement surgery is growing in popularity, but there is still a lot of misinformation out there, and it’s sometimes hard to figure out what facts are FACTS! Here are five things that you should know about disc replacement surgery before you have any operation on your spine: 1. Disc replacement surgery and disc arthroplasty surgery are the same thing. Also referred to as an “artificial disc” the implants used in these surgeries are designed to preserve motion in the spine after a discectomy (removal of the disc) and they have been shown to maintain motion and reduce the likelihood of degeneration at adjacent levels of the spine, something that often occurs in the years following a fusion. They are recommended for patients aged 18 – 70 years, but I, and other surgeons, have had excellent success in selected patients over the age of seventy. 2. Artificial discs are placed in the neck or back through the front of the spine (an anterior approach) after a damaged disc has been surgically removed to treat neck or back pain associated with radicular pain – the arm or leg pain caused by a “pinched” nerve. In the neck, this is the same approach we use for most disc surgeries, but in the lumbar spine the approach is often assisted by a vascular surgeon to limit the risk to the large vessels and other important structures in the abdomen. 3. Disc arthroplasty implants have been in development for over 40 years and have been available for patient care for nearly 2 decades. There are implants specifically designed for the cervical spine (neck) and for the lumbar spine (lower back). They have very specific applications – treatment of degenerated or herniated discs in otherwise healthy patients. There are no discs designed for the thoracic spine, and they are not intended to treat fractures, infections, scoliosis, or spondylolisthesis. And you can’t undo an old fusion and put in an artificial disc later! 4. Artificial disc replacement can be carried out as an outpatient surgery, and utilizes many minimally invasive techniques, but it is not “minor surgery”. When it comes to the spine, nothing is! The importance of surgeon experience and skill is reflected in the careful diagnosis and plan for treatment, and the skillful approach and placement of the implant. Surgeon experience with disc replacement procedures is important to the outcome here. Ask. 5. Disc replacements last a long time. How long? We don’t really know, because – unlike artificial hips and knees – we haven’t seen any of the ones we use today wear out. I’ve seen a suggestion that they will last 70 years, but that’s pure speculation! We have had the opportunity to observe patients in Europe who have had disc implants in place for 35 years without failures. And I have followed my own patients for more than 18 years without seeing any cases where the disc has worn out or deteriorated. There have been over 150 peer-reviewed publications of long-term trials and studies of total disc replacements, including investigational FDA trials, long-term follow-up studies, and large multicenter studies to ensure the safety and effectiveness of these implants. These studies have shown that, when used for the correct indications in the right patients, disc arthroplasty can provide significant advantages over traditional fusion procedures. They are not experimental or investigational, and their effectiveness is proven.
So, if you’ve been told you need to have a neck fusion, or a lumbar spine fusion, it’s ok to ask “is there another way to do this?”. You can learn more about disc replacement surgery, and other types of spine surgery and treatment, by checking out more sections of this website, or find me on Linkedin or Facebook at Robert McLain MD. Thanks!
5 Comments
When Does “Early” Spine Surgery Make Sense? When should you consider surgery for your back or neck? The old “rule of thumb” was that surgery for your back should be the very last thing you consider – when everything else has failed! Like most “rules of thumb” though, that’s only good advice some of the time. In certain situations, putting off surgery can lead to problems down the road, or be down-right dangerous. Here are FIVE CONDITIONS that may need surgery earlier rather than later:
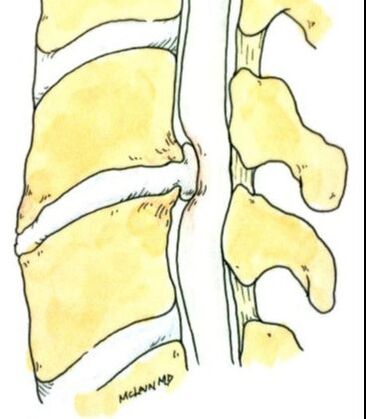
Conditions that destroy bone are usually more serious medical conditions, like tumors or infections, and require your Medical Specialists and your Spine Surgeon to work together. While the medical management is often the key to controlling the underlying disease, delaying surgery can lead to bone collapse and cause a much greater problem. Modern surgical techniques can provide stability with an overnight stay, keeping patients on their feet and minimizing pain during medical management. Spinal deformities should not be allowed to progress. A curvature of the spine or a slip of one vertebra relative to another that progresses in adulthood is most likely going to keep progressing! Early treatment will be less difficult and more successful than surgical reconstruction when the problem is severe. Nerve compression or spinal cord compression may be observed by your doctor for a while, but if symptoms of arm or leg pain are severe and persistent, or if any symptoms of spinal cord compression develop, there is no role for continued physical therapy or pain management. Spinal cord or nerve damage may become permanent, and surgery then - as a “last option” - may not do much good. Finally, there are some options available to patients with neck and back pain that just didn’t exist 20 years ago. Disc replacement, or disc arthroplasty surgeries lead to fewer re-operations and complications than traditional fusion procedures, and they protect the adjacent levels from degeneration often seen after fusion. However: total disc replacement operations PRESERVE MOTION, meaning that earlier surgery, while the spine is still mobile, is crucial. Waiting until the “last option” may mean there’s no motion left to preserve. And then, fusion is the right thing to consider. |
Details
AuthorI'm Dr. Rob McLain. I've been taking care of back and neck pain patients for more than 30 years. I'm a spine surgeon. But one of my most important jobs is... Archives
January 2024
Categories |
 RSS Feed
RSS Feed